Chemical Flea & Tick Treatments: What Every Pet Owner Should Know
In this guide I want to help all pet parents understand that common decisions can have huge impacts. One such decision is the chemicals that we use in or on our pets, for example whether to use parasite control, and today we will focus on fleas and ticks.
Fleas and ticks are not trivial. They can cause intense irritation, flea allergy dermatitis, secondary skin problems, anaemia in heavy infestations, and in some regions ticks may also transmit infectious disease. That is why parasite prevention matters. [1][2] I have experienced this first hand with some of my rescue animals. Its extremely distressing for your animal and you.
When it comes to flea and tick control, many pet owners are presented with two very extreme messages.
On one side, conventional advice often suggests that modern flea and tick medications are safe, effective, and should simply be used routinely every month. Regulatory bodies such as the AVMA and FDA do state that approved products can be safe and effective when used according to label instructions. [1][3]
On the other side, some natural-health messaging implies that if you feed raw, support the microbiome, or “boost immunity,” fleas and ticks will never be a problem. That is also misleading. Parasite pressure depends on many factors, including climate, geography, season, wildlife exposure, home environment, coat type, age, health status, and daily management. [2][4]
The truth often lies somewhere in between.
This article is not about fear. It is also not about blind trust. It is about helping pet parents make more informed, thoughtful decisions by understanding:
- how common flea and tick products actually work
- what their benefits and limitations are
- what the science (and real life experience from pet parents) say about side effects and environmental impact
- what natural prevention can and cannot realistically do
- when chemical treatment may still be justified
My position is simple: chemical flea and tick pesticides should only ever be used thoughtfully and sparingly, as a last resort or in very specific circumstances, not as a routine monthly default for every animal regardless of need.

The conventional veterinary perspective
Veterinary organisations generally recommend the use of regulated flea and tick preventatives because these parasites are real, common, and sometimes medically significant. The AVMA advises pet owners to use EPA-registered or FDA-approved products and follow label directions carefully [1]. The FDA also advises that flea and tick products can be used safely when directions are followed, while noting that product choice should take into account species, weight, age, and health status [3].
This approach is understandable from a ‘traditional’ perspective. Many of these products are convenient, fast-acting, and easier for owners than frequent combing, daily checks, and environmental control.
However, there is one basic fact that should never be forgotten:
All flea and tick medications are pesticides designed to kill living organisms.
That does not automatically mean they should never be used. It does mean they deserve proper respect, informed consent, and careful risk–benefit assessment.

How chemical flea and tick products actually work
Many flea and tick products sound similar, but they work in very different ways. Understanding this helps owners make more informed decisions.
1. Topical spot-on products
Examples include Frontline and Advantage. Please note brand names will vary in different countries.
These products are applied to the skin, usually at the back of the neck. The active ingredient spreads across the skin and coat via oils in the skin and hair. In other words, the pesticide does not remain in one small spot; the whole point is that it distributes over the animal’s body surface [1].
This is important because residues can then transfer to:
- hands when stroking the animal
- bedding, upholstery, carpets and car seats
- bathing water and wash water from bedding
- the wider environment
2. Oral systemic products
Examples include Bravecto, NexGard, Simparica and Credelio.
These products are swallowed and absorbed into the bloodstream. When a flea or tick bites and takes a blood meal, it ingests the compound and dies. This means the animal’s blood becomes the delivery route for the pesticide [5].
A common misunderstanding is that all oral tick products prevent bites. Many do not. Cornell’s guidance notes that oral isoxazoline products generally do not prevent tick attachment; they kill ticks after attachment, and the speed of kill is what matters. [5]
That distinction matters if owners assume oral products create a bite-proof barrier. They do not.
3. Pesticide collars
Examples include Seresto. There are many other products now on the market.
These collars slowly release active ingredients over time, spreading them across the skin and coat. Some collars can repel and kill ticks through contact, meaning the parasite may not need to bite first. [5][6]
However, collars also create prolonged, low-level pesticide exposure on the pet and in the home environment over weeks or months.
Common ingredients pet owners should recognise
| Product example | Common active ingredient(s) | Product type | Key points to know |
| Frontline | Fipronil | Topical | Highly toxic to aquatic invertebrates; detected in rivers in environmental monitoring studies [7] |
| Advantage | Imidacloprid | Topical | Neonicotinoid insecticide; also detected in rivers and associated with aquatic risk [7] |
| Bravecto | Fluralaner | Oral | Isoxazoline class; FDA warns this class has been associated with neurologic adverse events in some pets [8] |
| NexGard | Afoxolaner | Oral | Isoxazoline class; same FDA neurologic warning applies [8] |
| Simparica | Sarolaner | Oral | Isoxazoline class; same FDA neurologic warning applies [8] |
| Seresto | Imidacloprid + Flumethrin | Collar | Long-lasting collar; may repel ticks through contact but also creates prolonged environmental exposure [5][6] |
Reported adverse events do not mean every pet will react badly. However, they do clearly demonstrate that these products are biologically active substances, not neutral interventions.
It is also critical to understand that official adverse event statistics almost certainly underestimate the true number of reactions.
Veterinary pharmacovigilance systems rely heavily on voluntary reporting, and research has consistently shown that a large proportion of adverse drug reactions in animals are never formally reported. Recent evidence suggests that the majority of suspected adverse reactions in veterinary practice go unreported, meaning published figures likely represent only a fraction of real-world cases.[18] [19]
There are several reasons for this underreporting:
-
reporting is often not mandatory for veterinary professionals [20]
-
mild or delayed reactions may not be recognised as drug-related
-
time constraints and administrative burden reduce reporting rates
-
pet owners may share experiences informally (e.g. online communities) rather than through official channels
Regulatory bodies themselves acknowledge important limitations in adverse event databases. For example, the FDA states that adverse event reporting systems are designed as early warning tools, and that the data collected cannot be used to determine true incidence rates.[21] [22]
In practical terms, this means that while official figures are useful for identifying potential safety signals, they should not be interpreted as a complete picture of risk.
When combined with growing anecdotal reports from pet owners and veterinary practitioners, a more cautious and informed approach to routine pesticide use becomes not only reasonable, but necessary.
Side effects and why susceptibility varies between animals
Not every animal responds to pesticides in the same way. Just as people vary in how they respond to medications, pets vary too.
Factors that can influence susceptibility include:
- age
- body size
- baseline health
- existing liver, skin, or immune challenges
- total chemical load from other sources
- diet and microbiome health
- stress levels
- breed and genetics
- environmental exposure to fleas and ticks
One recognised genetic factor is the MDR1 mutation. Washington State University explains that dogs with this mutation may have severe reactions to certain drugs because of altered drug transport across protective barriers in the body. Breeds commonly affected include Collies, Australian Shepherds, Shetland Sheepdogs and related mixes. [9][10]. I have had my mix breeds tested for this mutation – if in doubt have your dogs tested – it could save their life.
It is important to say this accurately: the MDR1 mutation does not automatically make a dog sensitive to every flea product, but it is a clear example of why blanket statements such as “these products are safe for all pets” are too simplistic.
The FDA has also issued a specific alert for the isoxazoline class, noting reports of neurologic adverse reactions including tremors, ataxia and seizures in some dogs and cats. [8]
These chemicals do not stay neatly on the pet
One of the biggest misconceptions about flea and tick pesticides is that they remain isolated to the animal.
They do not.
Topical products can transfer to hands, furniture, bedding, carpets, and wash water. [1][11] Oral products circulate through the animal’s body and are later excreted via urine and faeces. [12]
This means flea and tick chemicals do not just affect the pet. They can also enter:
- the household environment
- wastewater systems
- soil and garden environments
- rivers and lakes
- wildlife habitats
That does not mean every treated pet is in immediate danger. It does mean these compounds should not be thought of as staying politely contained.
Environmental impact: the evidence is growing
This is one of the most important parts of the conversation, because the environmental evidence is now substantial.
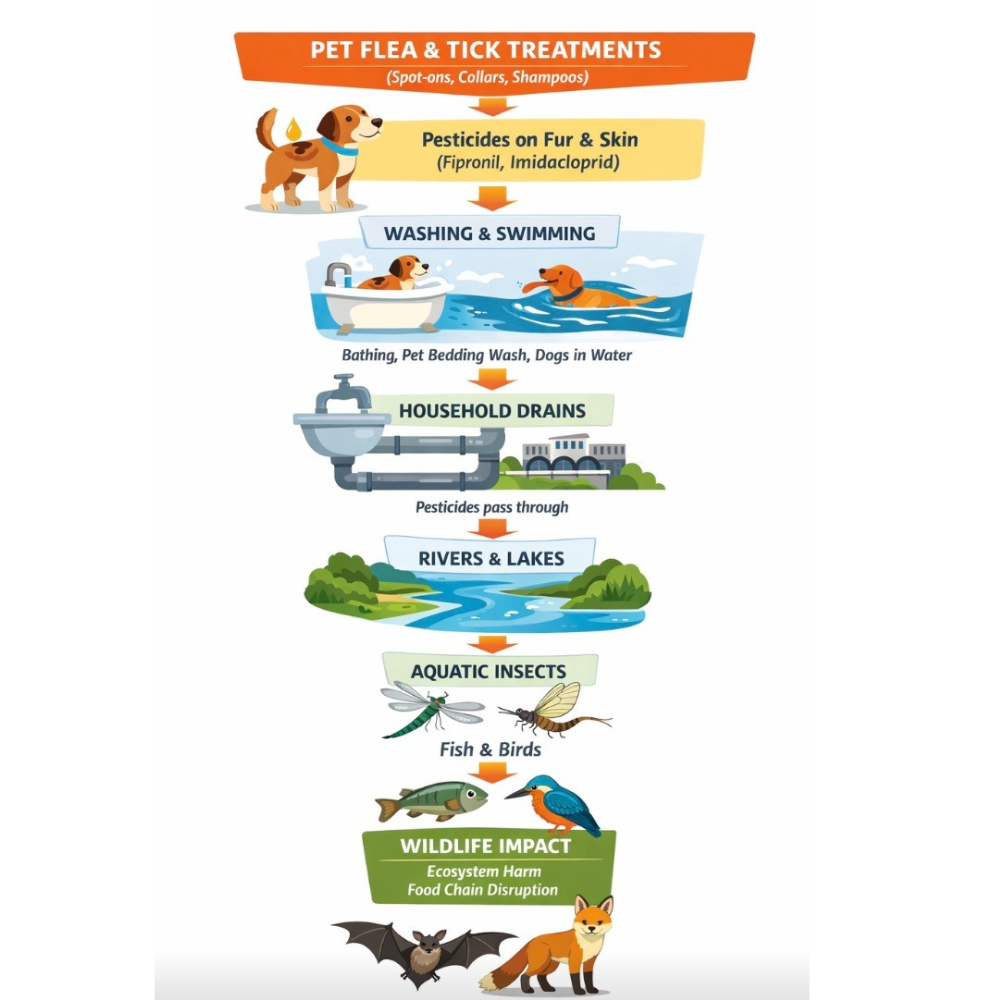
A 2021 peer-reviewed paper found that fipronil, its metabolites, and imidacloprid were common in English rivers, often at concentrations above accepted safety thresholds for aquatic ecosystems. The authors concluded that veterinary flea products were a plausible and important source of this contamination. [7]
A 2024 follow-up study looked specifically at “down-the-drain” pathways from treated dogs and found that bathing dogs, washing pet bedding, and even owners washing their hands after applying spot-ons could contribute to wastewater contamination. The researchers estimated these pathways could account for a substantial share of the measured pollution. [11]
A 2025 study on dogs swimming after treatment found that fipronil and imidacloprid were detected in 100% of swimming samples from treated dogs in that study, confirming that swimming is a real pathway for pesticide release into water. [13]
The problem does not stop at waterways. A 2025 study of blue tit and great tit nests found fipronil in 100% of nests tested, and imidacloprid and permethrin in the majority. Higher insecticide levels were linked with increased offspring mortality. The study concluded that the most common insecticides found in nests were veterinary products, likely transferred in fur used to line nests. [14]
These chemicals are now widely detected in UK rivers, which ultimately feed into our drinking water systems. Given that conventional treatment processes are not designed to fully remove such compounds, this raises important questions about how much is ultimately removed — and how much may persist in the wider water cycle. Absence of routine testing does not equal absence of exposure.
Simple diagram: how pet flea chemicals move through the environment
Why flea problems can seem worse than ever
Many pet owners feel they are using more products yet still struggling more. Several factors may explain this.
Longer parasite seasons
Warmer conditions can extend flea and tick activity in many regions. [2][15]
Wildlife exposure
Pets living near woodland, sandy soil, farmland, deer, foxes, rodents, or feral animal populations are likely to face far greater exposure than urban pets. [2][4]
Indoor conditions
Fleas spend most of their life cycle off the animal. CDC explains that eggs, larvae and pupae develop in the environment, and pupae are protected by cocoons that can survive for days or weeks until conditions are right. [4] Heated homes, carpets and soft furnishings make it much easier for fleas to persist year-round.
Resistance
Resistance is a real biological phenomenon. A major review found that flea resistance has developed to several older insecticide classes, including carbamates, organophosphates and pyrethroids. [16] Genetic mutations associated with pyrethroid resistance have also been identified in cat fleas. [17]
At the same time, the review notes that not all treatment failure is true resistance; poor compliance, environmental reinfestation, and failure to treat the full flea life cycle can also explain why products appear to stop working. [16] That balanced point is important.
Generally Lower Resistance in our Pets
There’s another piece of the puzzle that rarely gets discussed.
Many of our pets today are simply not as resilient as they once were.
With increasing exposure to:
-
processed diets
-
medications and chemical treatments
-
environmental toxins
-
chronic stress
we’re seeing more animals with compromised microbiomes and immune function.
From a terrain perspective, this creates the perfect conditions for parasites to thrive.
Fleas and ticks are opportunistic — and while exposure is always a factor, animals with depleted internal balance often struggle more with:
-
recurring infestations
-
exaggerated reactions
-
difficulty clearing parasites naturally
This is why simply “killing the fleas” is often not enough.
Without addressing the underlying terrain, the cycle can continue. – Dr Judy Morgan and I discuss this in this video: https://youtu.be/uUZ45TrxEzA?si=VIe7IM6owQXtQ2pl
Myth-busting natural prevention
Natural prevention is often misunderstood too.

Diet absolutely matters. Skin health, immune function, microbiome resilience, and overall vitality all influence how well an animal copes. But diet alone is not a magic shield against environmental exposure. My dogs are all raw fed – and yes they get fleas!
A dog living in woodland, with wildlife passing through the garden and sandy soil underfoot, is dealing with a very different parasite challenge from a dog living mainly on paved streets in a city flat. [2][4]
So the honest message is this:
- natural prevention can be very helpful
- natural prevention is best used as a layered strategy
- natural prevention requires consistency
- natural prevention is not the same as “do nothing and hope for the best”
What natural prevention can do well
Natural strategies can help reduce parasite pressure while supporting overall health and lowering chemical burden.
Foundational prevention
- balanced, species-appropriate nutrition
- microbiome support
- good coat and skin condition
- regular movement and sunlight
- stress reduction
Practical prevention
- flea combing regularly
- daily tick checks during risk periods
- washing bedding frequently
- vacuuming carpets, upholstery and car interiors
- checking after woodland or high-risk walks
Natural deterrents
- carefully chosen herbal or essential oil sprays
- beneficial nematodes in the garden
- environmental powders or sprays used knowledgeably
- collars or tags only where ingredients and manufacturing quality are clear
- Natural does not automatically mean safe. Essential oils must be species-appropriate and properly diluted, especially around cats. Quality control also varies greatly, particularly with vague “natural flea collars” sold online.

Treat the environment, not just the pet. This is one of the most important practical points for owners to understand.
Fleas are not mainly a problem on the animal. The CDC flea life cycle shows that much of the flea population exists off-host as eggs, larvae and pupae in the environment. [4]
If you only focus on the animal, you may be missing the bigger part of the problem.
Consider:
- washing bedding more frequently during risk periods
- vacuuming thoroughly, especially edges, cracks and upholstery
- cleaning car seats and transport crates
- using beneficial nematodes in the garden
- improving sunlight and dryness in outdoor resting areas where possible
- paying attention to wildlife traffic, visiting dogs, kennels and grooming environments
By addressing the environment, you are far more likely to break the flea life cycle at its source.
I cover individual strategies for your pets in my consults – these points apply to everyone, but specific support for your animals will need a bespoke plan. Products vary in different countries etc.
When chemical treatment may still be justified
A balanced article should say this clearly: there are situations where chemical treatment may be justified. The decision should not be taken lightly BUT sometimes it is needed. The key is the support you give when chemicals are used, and again I stress only using when absolutely necessary:
For example:
-
- a severe flea infestation
- flea allergy dermatitis causing significant suffering
- a rescue animal arriving heavily parasitised
- very high tick pressure in a region where disease risk is significant
- repeated failure of good environmental and natural management
- In these situations, the better question is not:“Chemicals or no chemicals?”It is:“What is the lowest-risk strategy that still protects this individual animal in this environment?”
That is a far more thoughtful framework than automatic monthly dosing for life.
If chemicals must be used, how to reduce the burden?
If you do decide that a chemical flea or tick product is necessary, try to use it strategically rather than casually.Helpful principles include:
- avoid stacking multiple chemical exposures at the same time where possible
- do not combine flea treatment with other non-urgent exposures unnecessarily
- increase environmental cleaning to reduce the need for repeat use
- support nutrition, hydration and recovery afterwards
- review other chemicals in the home and garden to reduce total toxic load
Supportive measures many owners explore include:
- soil-based probiotics
- excellent home-prepared or whole-food nutrition
- gentle liver support, such as milk thistle where appropriate
- consistent exercise and stress reduction
- detox-support products chosen carefully and individually (seek professional advice)
This is also where personalised support can make a big difference, because the best strategy depends on the animal, the household, and the level of exposure.
A simple decision framework
Step 1 — Assess risk
Ask:
- Do you live near woodland, wildlife or sandy soil?
- Is your pet outdoors a lot?
- Are ticks common where you live?
- Is flea pressure seasonal or year-round?
Step 2 — Assess the animal
Ask:
- Is my pet young, elderly, sensitive, or chronically unwell?
- Has my pet recently had other medications or vaccines?
- Is my breed one that may have relevant sensitivities, such as MDR1? [9]
Step 3 — Start with prevention
Focus first on:
- nutrition
- microbiome health
- grooming including daily flea comb
- tick checks
- environmental management
- natural deterrents where appropriate
Step 4 — Intervene early
If you begin to notice fleas, flea dirt, ticks, itching, or early signs of an infestation, act promptly with environmental cleaning and layered natural support rather than waiting until the situation escalates.
Step 5 — Use chemicals only when genuinely needed
If the burden is high, the animal is suffering, or the local disease risk is substantial, strategic temporary chemical use may be justified.
Step 6 — Support recovery
Before, during and after chemical use, focus on rebuilding resilience and reducing future need through environmental control, microbiome support, good nutrition and reduced chemical stacking.
My balanced recommendations
If I had to summarise this entire topic simply, it would be this:
- Assess each animal individually.
- Do not assume routine monthly pesticides are the only responsible option – they should be a last resort / used in exceptional circumstance.
- Build strong health foundations and manage the environment first.
- Use natural prevention consistently, not casually.
- Reserve chemical intervention for situations where it is truly needed.
- If chemicals are used, support the animal before, during & afterwards and reduce other exposures.
Fleas and ticks are real. But protecting our animals does not have to mean automatic lifelong pesticide use.
A more thoughtful approach protects not only our pets, but also:
- their long-term health
- our homes
- the soil and water around us
- wildlife and ecosystems
Healthy animals and healthy environments ultimately go hand in hand.
Products I use:
Need personalised help?
If you would like help creating a parasite prevention strategy tailored to your animal and environment, you can learn more about my consultations here:
-
- Consultations:
https://www.catherineedwards.life/holistic-consults/
- Consultations:
Helpful product links
UK / Europe probiotics:
https://www.catherineedwards.life/product/microbz/
Use code CATHERINEEDWARDS for 20% off
USA / Canada support:
https://www.catherineedwards.life/product/dr-dobias-supporting-natural-dog-wellness/
| Ref. | Citation | Link |
|---|---|---|
| [1] | American Veterinary Medical Association (AVMA). Safe use of flea and tick preventive products. | View source |
| [2] | Centers for Disease Control and Prevention (CDC). About fleas. | View source |
| [3] | U.S. Food and Drug Administration (FDA). Safe Use of Flea and Tick Products in Pets. | View source |
| [4] | Centers for Disease Control and Prevention (CDC). Flea Lifecycles. | View source |
| [5] | Cornell University Riney Canine Health Center. Flea and tick prevention. | View source |
| [6] | Elanco. Seresto Flea & Tick Control Collar. | View source |
| [7] | Perkins, R. et al. (2021). Potential role of veterinary flea products in widespread pesticide contamination of English rivers. | View source |
| [8] | FDA. Fact Sheet for Pet Owners and Veterinarians about Potential Adverse Events Associated with Isoxazoline Products. | View source |
| [9] | Washington State University Veterinary Clinical Pharmacology Laboratory. MDR1 in dogs. | View source |
| [10] | Washington State University Veterinary Hospital. Is your pet at risk of an adverse reaction to common drugs? | View source |
| [11] | Perkins, R. et al. (2024). Down-the-drain pathways for fipronil and imidacloprid applied as spot-on parasiticides to dogs. | View source |
| [12] | Diepens, N.J. et al. (2023). Pet dogs transfer veterinary medicines to the environment. | View source |
| [13] | Perkins, R. et al. (2025). Swimming emissions from dogs treated with spot-on fipronil or imidacloprid. | View source |
| [14] | de Montaigu, C.T. et al. (2025). High prevalence of veterinary drugs in bird’s nests. | View source |
| [15] | Centers for Disease Control and Prevention (CDC). Ticks. | View source |
| [16] | Rust, M.K. (2016). Insecticide resistance in fleas. | View source |
| [17] | Bass, C. et al. (2004). Identification of mutations associated with pyrethroid resistance in the cat flea. | View source |
| [18] | BSAVA (2024). Majority of suspected adverse drug reactions in veterinary medicine are unreported. | View source |
| [19] | Davies, H. et al. (2024). Recording of suspected adverse drug reaction reporting in veterinary practice. | View source |
| [20] | RCVS / Veterinary guidance (reporting obligations and limitations). | View source |
| [21] | FDA Center for Veterinary Medicine. Adverse Event Reporting System – limitations. | View source |
| [22] | Monteiro et al. (2025). Challenges in veterinary pharmacovigilance and underreporting. | View source |